Urgently Needed, A Global Response to the Zika Virus
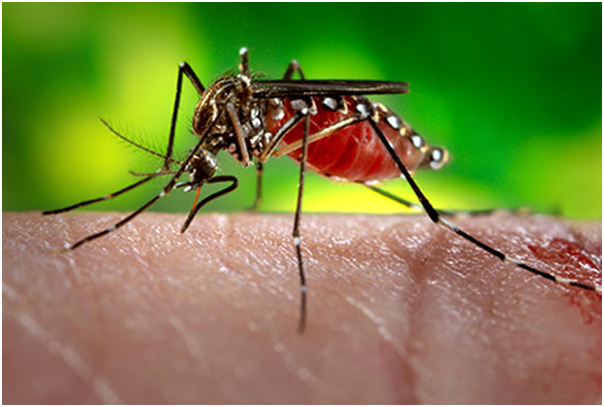
The vector that transmits the Zika virus
Global concerns about a new viral pandemic have started making headlines barely weeks after resolution of the Ebola epidemic in West Africa. The virus responsible for panic buttons being pressed, with the WHO declaring a ‘public health emergency of international concern’, is the Zika virus. Threats to health at a global scale in the form of epidemics caused by viruses are now too frequent to view these threats as one-off events. There are structural reasons why we need to be prepared for more such challenges to global health.
The Zika virus is so named because it was first isolated in the Zika forest of Uganda. Interestingly the virus was first isolated not in humans, but in an infected Rhesus monkey in 1947. Human infections were subsequently recorded around 1952 in Uganda and Tanzania. The Zika virus, thus, has been known to be around for decades and appears to have jumped species to affect human populations. Zika virus infections have been reported in the tropical band across Africa, and parts of Asia and South East Asia. There have been outbreaks of local epidemics, including one in the urban areas of Gabon in 2007.
The Zika virus belongs to the Flavivirus group of viruses, the same group that cause Dengue fever and Yellow fever. It is transmitted by the Aedes mosquito, with the Aedes aegypti species being the most implicated. The Aedes is now understood to be the most prevalent mosquito in the world and also transmits other viral infections to humans, such as Dengue fever and Chikungunya.
The infection causes relatively mild symptoms in the affected host and includes fever, headache and body ache and rashes. Typically the symptoms have been described as similar but milder to those in Dengue infections, without the latter’s most serious complications like severe bleeding. The infection has an incubation period (i.e. the period between infection and the expression of symptoms) of 3-10 days and a patient remains infective for a week to ten days after the symptoms appear. Not everyone who is infected show symptoms, and it is estimated that of all patients infected only about 20% exhibit some symptoms. Experience till now suggest that the infection is self limiting, and rarely if ever requires hospitalization.
There are no specific medicines for the infection and only medicines to treat the symptoms of fever and pain, such as paracetamol, are recommended. Patients are cautioned against taking non-steroidal anti inflammatory drugs such as aspirin, ibuprofen and diclofenac as they worsen bleeding tendencies in dengue patients, given that the symptoms of Zika infection and dengue are very similar. Currently no rapid diagnostic tests are available to confirm Zika infection. Molecular biology based confirmatory tests for Zika infection take considerable time, are expensive and few laboratories have the facilities to do these diagnostic tests.
Infection by the Zika virus was practically unknown in the Americas till very recently. It is now conjectured that the virus travelled from the Asian region, through French Polynesia, including for example Tahiti, to Mexico and then to Brazil and other counties in Latin America sometime in 2015. In Brazil, primarily in the 3 North-East districts, a sharp rise in febrile illnesses was noticed in 2015. The causative virus was identified as the Zika virus. This route of transmission of the infection – from Asia via French Polynesia – appears likely as the Zika virus affecting Brazil and other countries in the region such as Colombia, appears more closely related to the Asian variant of the Zika virus.
If this was the entire story, there wouldn’t have been cause from any great concern given the relatively mild symptoms. Alarm bells started ringing when a spike in the number of cases of microcephaly was detected in the regions in Brazil affected most by the Zika virus. Microcephaly is a condition where babies are born with unusually small skulls. It is a developmental defect and is usually also associated with serious nervous system disorders – including deficiencies in mental functions and muscular weaknesses of varying degrees. There is no remedy available after a baby is so affected.
In the affected districts of Brazil the reports of microcephaly were followed up, and till date several hundred established cases that are new have been recorded. Microcephaly is known to occur sporadically in any population, but the rate of incidence detected in Brazil is much higher than normally expected. Further tests have shown that the Zika virus is able to cross the placental barrier in a pregnant woman infected by the Zika virus, that is the virus is able to enter the sac containing the baby and is able to infect the baby. As yet, while the correlation between a rise in microcephaly cases and the incidence of Zika virus infection is strong, direct causality has not been proved. However the possibility that Zika virus infection in pregnant women can lead to microcephaly appears very strong. In fact Zika virus infections also show a strong correlation with another serious illness – called Guillain–Barré syndrome. This is a disease which is known to follow viral infections and leads to paralysis of muscles, sometimes including almost the entire body. It is a self limiting disease and patients take a few months to recover, and usually recovery is complete. However during the phase when the patient is paralysed intensive supportive measures are required, often in a hospital setting.
Attention has been focused in recent months to, on one hand prove conclusively that Zika virus infection during pregnancy causes a rise in microcephaly cases, and on the other in attempting to ensure that pregnant women are shielded from infection by the virus. The latter is a virtually impossible task for women living in areas where there is an ongoing Zika virus epidemic – it is estimated for example that over 5,00 women are pregnant in the Zika affected regions of Colombia. As we discuss earlier a large proposition of those infected may not exhibit symptoms, so theoretically a pregnant woman may not exhibit any symptoms of the infection and yet be at risk of giving birth to a baby with microcephaly. There are no drugs available that can prevent infection and diagnosis is difficult and expensive, so most women have no means of either protecting themselves or of knowing if they are at risk. Microcephaly can be detected by doing an ultrasound examination, but conclusive proof is available relatively late in pregnancy, usually too late to consider an abortion.
Given these complexities the only immediate recourse appears to be to advise woman to avoid getting pregnant if they live in a region currently affected by the Zika virus or if they have recently visited such a region. Clearly complete compliance with such an advisory is very difficult. Many countries, including Brazil and the United States (for travelers) have issued such advisories and women are being asked to avoid pregnancy at least three weeks after they have left a Zika affected region. Obviously this does not work for women who live in an affected area, especially those living in the affected districts of Brazil and other neighbouring Latin American countries. For such women the advise being offered is that they should postpone pregnancy indefinitely till a vaccine for the virus is available.
The problem is further compounded by reports that the virus, in addition to being transmitted through mosquito bites, can also be transmitted through blood transfusion from infected individuals and also through sexual intercourse. The former route of possible transmission imposes extra burden on health systems to test for Zika infection before blood or other blood products are transfused. The risk of a sexual route of transmission imposes uncertainty as regard the infective period. While the virus is likely to disappear after a week to 10 days from the onset of symptoms, or about 20 days after a person is infected, it could continue to be found in the testes of infected individuals for many weeks (thus making them capable of passing on the infection for longer periods).
The Zika story needs also to be understood in the broader context of transmission of communicable diseases in a globalised world. Globalisation has contributed vastly to the mobility of populations, thus multiplying the risk of new infections appearing in regions that did not harbor them. A question that remains unanswered is why microcephaly cases did not see a rise in regions in Africa and Asia, where the virus is known to have existed for decades. Partially, this might have to do with less than robust reporting system in these countries. An additional factor could be that the infection spread much more slowly in these regions, taking decades to affect a significant proportion of the population. This probably also allowed the development of some form of immunity, thus providing at least partial protection against the infection. In contrast the relatively sudden appearance of the virus in a population that was never exposed earlier (like it happened in Brazil) allowed the infection to spread much faster and in the absence of any immunity against the virus in the population. This is a generic problem that public health systems will need to contend with and also explains the rapid spread of many viruses as global pandemics or regional epidemics in the past decade – the avian flu virsus, the H1N1 or swine flu virus, and the Ebola virus.
There are several drivers of recent instances of global health challenges posed by viral pandemics and epidemics. Mobility of populations is clearly a driver, compounded by the generally poor access to health care services for migrant populations. Further we have new hybrid viruses appearing in the huge food processing factories, which multiply the chances of human animal interactions. Both the bird flu and the swine flu viruses jumped species and started affecting humans by mutating in conditions suitable for their survival and multiplication. Human animal interface is also increasing as indigent populations are being forced deeper into forested areas. This is likely to have been a reason why the Ebola virus, traditionally known to infect the fruit bat, started infecting humans. We may yet see evidence of a similar phenomenon being responsible for the Zika virus embracing a human host, while traditionally it was an infection largely confined to the monkey population. Climate change is also playing a role – warmer climates are leading to disease vectors such as mosquitoes spreading to new areas.
Unfortunately, while the drivers of the new epidemics are global, we are failing to mount a global response.
International health co-operation has been converted to ‘security’ responses by the rich and powerful countries. Clampdowns and restrictions, aimed at sanitizing the rich countries, just do not work. Simultaneously disease surveillance by international organisations – prominently the World Health Organisation -- is at a new low.
The US and other developed countries have, in a planned manner, choked international bodies such as the WHO and other UN agencies, of resources. Instead they foist on the global populace institutional mechanisms that are not driven by sovereign nation states, but rather by private interests. We thus have global partnerships taking over the space ceded by UN agencies – for example the Global Fund for HIV, TB and Malaria and the Global Alliance for Vaccines and Immunisations (GAVI).
Both these powerful global partnerships were situated outside the WHO in order to provide a voice to private foundations (prominently the Gates Foundation), private corporations and rich donor countries. While new knowledge will need to be the cornerstone of the battle against the new challenges on global health, this knowledge is sought to be sequestered in a few hands and to be utilized for private interests or the interests of a few powerful countries. GAVI, for example, has done too little to transfer technology and build capacity in Low and Middle Income countries for vaccine research and vaccine development.
The H1Ni pandemic alert a few years back was followed by the unsavory spectacle of almost the entire stock of vaccines against H1N1 being bought up in advance by a few rich countries. If the pandemic had actually transpired vaccine availability in Low and Middle Income countries would have taken several years. The only long term solution to the Zika crisis is an effective vaccine – conceivably about a year away.
We have no guarantee that the H1N1 fiasco will not be repeated, and that countries such as India will not have to wait for years to access the vaccine. The same is likely to be true for rapid diagnostic kits for diagnosis of Zika infection. All countries are at a risk of the Zika virus spreading, but the current global power relations ensure that remedies will be available first to the rich and the powerful.
The globe’s responses to viral epidemics and pandemics show a mirror to the inequity embedded in the system of global governance today. We cannot anymore fight this battle virus by virus.
A global response will need to address the structural failures of globalization – where it unleashes new challenges at a global scale but forces a response that is not truly international in character.
(Courtesy: NewsClick)



